Cardiac Muscle and the Mammalian Heart
The mammalian heart is a four-chambered pump built from a specialized type of muscle found nowhere else in the body. Understanding how cardiac muscle works, how the heart's electrical system coordinates contraction, and how the cardiac cycle moves blood in one direction are central to this topic.
Structure and Function of Cardiac Muscle
Cardiac muscle is striated (it has the same sarcomere organization as skeletal muscle, with sliding filaments of actin and myosin) but it's involuntary, meaning it contracts without conscious control.
What makes cardiac muscle unique:
- Intercalated discs are specialized junctions between cardiac muscle cells. They contain gap junctions that allow electrical impulses to pass rapidly from cell to cell, so the heart contracts as a coordinated unit rather than one fiber at a time.
- Autorhythmic cells in the sinoatrial (SA) node spontaneously generate action potentials, making the SA node the heart's natural pacemaker. You don't need a signal from the brain to keep your heart beating.
- The atrioventricular (AV) node receives impulses from the SA node but introduces a brief delay. This delay is critical because it gives the atria time to finish contracting and push blood into the ventricles before the ventricles contract.
- Cardiac muscle has a long refractory period compared to skeletal muscle. This prevents tetanic contraction (sustained, locked-up contraction), which would stop the heart from filling between beats.
- Coronary circulation is the heart's own blood supply. The coronary arteries branch off the aorta and deliver oxygen and nutrients directly to the heart muscle tissue. A blockage here is what causes a heart attack.
Stages of the Cardiac Cycle
The cardiac cycle is the sequence of contraction and relaxation that occurs with each heartbeat. It has three main stages:
-
Diastole (relaxation phase)
- Both the atria and ventricles relax.
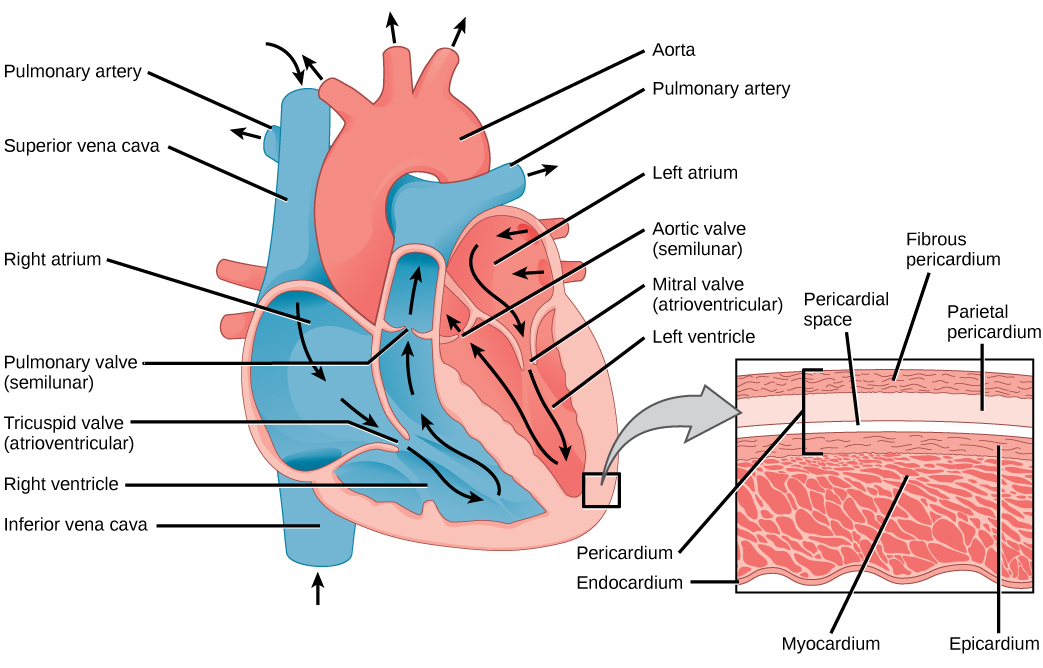
- The AV valves (tricuspid on the right, mitral/bicuspid on the left) open, allowing blood to flow passively from the atria into the ventricles.
- The semilunar valves (pulmonary and aortic) are closed, preventing blood from flowing back into the ventricles from the arteries.
-
Atrial systole (atrial contraction)
- The atria contract, pushing the remaining blood into the ventricles. Most ventricular filling actually happens during diastole; atrial systole tops it off.
- AV valves remain open; semilunar valves remain closed.
-
Ventricular systole (ventricular contraction)
- The ventricles contract with enough force to push blood out of the heart.
- The AV valves snap shut (this produces the first heart sound, "lub"), preventing backflow into the atria.
- The semilunar valves open, sending blood into the pulmonary artery (right ventricle) and the aorta (left ventricle).
- When the ventricles relax again, the semilunar valves close (producing the second heart sound, "dub").
Unidirectional flow depends entirely on the coordinated opening and closing of these valves. Oxygenated blood is pumped to the body through the systemic circuit, while deoxygenated blood is pumped to the lungs through the pulmonary circuit for gas exchange.
Blood Vessels and Circulation
The blood vessels form a closed network that carries blood away from the heart, delivers it to tissues, and returns it. The three main vessel types differ in structure because they serve very different functions.
Types of Blood Vessels
Arteries carry blood away from the heart.
- They have thick, elastic walls that can withstand the high pressure generated by ventricular contraction.
- A layer of smooth muscle in the arterial wall allows vasoconstriction (narrowing) and vasodilation (widening), which helps regulate blood pressure and direct blood flow to where it's needed.
- Arteries branch into smaller arterioles, which deliver blood to capillary beds.
Capillaries are where the real work of the circulatory system happens: exchange of gases, nutrients, and wastes between blood and tissues.
- Their walls are only one cell thick (simple squamous endothelium), which allows efficient diffusion of , , glucose, and other molecules.
- The body contains a vast network of capillaries, maximizing the surface area available for exchange.
Veins carry blood back to the heart.
- Their walls are thinner and less elastic than arteries because blood pressure in veins is much lower.
- Veins contain one-way valves that prevent backflow. Skeletal muscle contractions around veins also help push blood back toward the heart.
- Small venules collect blood from capillary beds and merge into larger veins.

Blood Flow Path
The two circuits work in series:
- Systemic circuit: Left ventricle Aorta Arteries Arterioles Capillaries Venules Veins Vena cava Right atrium
- Pulmonary circuit: Right ventricle Pulmonary artery Lungs (gas exchange) Pulmonary veins Left atrium
Notice that the pulmonary artery carries deoxygenated blood and the pulmonary veins carry oxygenated blood. This is a common exam question: arteries and veins are defined by direction of flow (away from or toward the heart), not by oxygen content.
Cardiovascular System Function and Monitoring
The cardiovascular system distributes , nutrients, and hormones to every tissue in the body while removing metabolic wastes like .
- Blood pressure is determined by two main factors: cardiac output (how much blood the heart pumps per minute) and the diameter of blood vessels. Vasoconstriction raises blood pressure; vasodilation lowers it.
- Hemoglobin, the iron-containing protein in red blood cells, binds in the lungs and releases it in the tissues where oxygen concentration is low.
- An electrocardiogram (ECG/EKG) records the electrical activity of the heart through electrodes on the skin. The P wave corresponds to atrial depolarization, the QRS complex to ventricular depolarization, and the T wave to ventricular repolarization. Abnormal patterns help diagnose arrhythmias, heart attacks, and other cardiac conditions.