Bone Structure and Function
Bone is living, dynamic tissue that provides structural support, protects organs, stores minerals, and produces blood cells. Understanding bone means knowing its cell types, its composition, and how it develops and remodels throughout life.
Types of Human Skeletal Bones
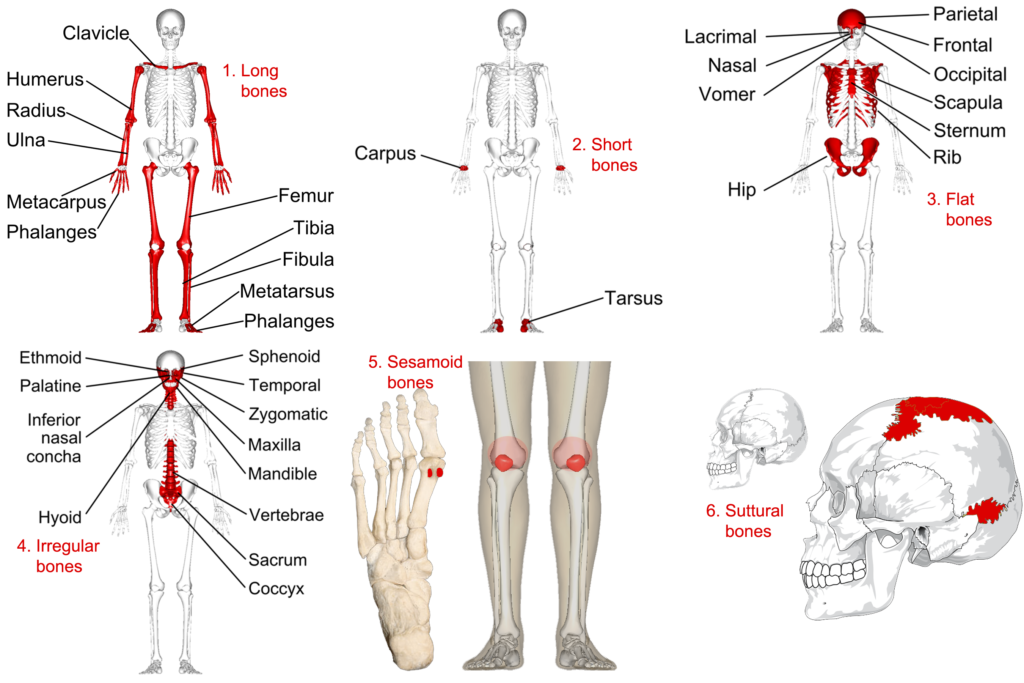
The human skeleton contains five categories of bone, classified by shape. Each shape reflects a different functional role.
- Long bones are longer than they are wide, with a shaft (diaphysis) and two ends (epiphyses). They act as levers for movement. Examples: femur, humerus, radius, ulna, metacarpals, metatarsals.
- Short bones are roughly cube-shaped and provide stability with limited movement. They're found in the wrist (carpals) and ankle (tarsals).
- Flat bones are thin and broad. They protect underlying organs and provide large surface areas for muscle attachment. Examples: skull bones, scapulae, ribs, sternum.
- Irregular bones have complex shapes that don't fit the other categories. They often protect internal structures. Examples: vertebrae, sacrum, coccyx.
- Sesamoid bones are small bones embedded within tendons, where they reduce friction and protect the tendon from wear. The patella (kneecap) is the largest sesamoid bone.
Bone Cells and Their Functions
Three main cell types work together to build, maintain, and remodel bone tissue.
Osteoblasts are the bone-building cells. They secrete osteoid, which is the unmineralized protein matrix of bone (mostly collagen). Once minerals deposit onto the osteoid, it hardens into bone. When an osteoblast becomes completely surrounded by the matrix it produced, it matures into an osteocyte.
Osteocytes are the most abundant bone cells. They sit within small spaces called lacunae and extend long projections through tiny channels called canaliculi. This network lets osteocytes communicate with each other and sense mechanical stress on the bone. That mechanical sensing is what triggers remodeling in response to the forces your body experiences.
Osteoclasts are large, multinucleated cells that break down (resorb) bone. They secrete acids and enzymes that dissolve both the mineral and organic components of bone matrix, releasing stored calcium and phosphate into the blood. Osteoclast and osteoblast activity must stay in balance to maintain healthy bone density.

Bone Composition and Structure
Bone gets its unique properties from a combination of organic and inorganic materials.
- The organic component is primarily collagen fibers, which give bone its flexibility and resistance to tension. Without collagen, bone would be brittle and shatter easily.
- The inorganic component is mainly hydroxyapatite, a crystalline calcium phosphate mineral (). This mineral gives bone its hardness and compressive strength.
The combination of collagen and hydroxyapatite is what makes bone both strong and somewhat flexible.
At the tissue level, compact bone (the dense outer layer) is organized into cylindrical units called osteons (Haversian systems). Each osteon has concentric rings of bone matrix (lamellae) surrounding a central Haversian canal that carries blood vessels and nerves. Spongy bone (cancellous bone), found at the ends of long bones and in the interior of flat bones, has a lattice-like structure of bony struts called trabeculae that resist stress while keeping the bone lightweight.
Other key structures:
- The periosteum is a tough fibrous membrane covering the outer surface of bone. It contains blood vessels, nerves, and osteoblasts important for bone growth and repair.
- Bone marrow fills the internal cavities. Red marrow produces blood cells (hematopoiesis), while yellow marrow stores fat. In adults, red marrow is mainly found in flat bones and the epiphyses of long bones.
Bone Development and Growth
Intramembranous Ossification
This process forms flat bones (such as the skull bones). No cartilage template is involved.
- Mesenchymal cells (embryonic connective tissue cells) cluster together and differentiate directly into osteoblasts.
- Osteoblasts secrete osteoid, which then mineralizes to form small islands of bone called trabeculae.
- These trabeculae merge, and additional bone is added to the surface through appositional growth (osteoblasts depositing new layers on existing bone).
- The periosteum forms around the outer surface, and compact bone eventually replaces the outer trabecular bone.
Endochondral Ossification
This process forms long bones and most other bones in the body. It starts with a cartilage model that is gradually replaced by bone.
- Mesenchymal cells differentiate into chondrocytes, which secrete cartilage matrix to form a hyaline cartilage model shaped like the future bone.
- Chondrocytes in the center of the model hypertrophy (enlarge), and the surrounding matrix calcifies. The chondrocytes then die, leaving cavities.
- A periosteal bud (blood vessels and osteoblasts) invades the cavities, forming the primary ossification center in the diaphysis.
- Osteoblasts deposit osteoid on the remnants of calcified cartilage, and this osteoid mineralizes into true bone.
- Secondary ossification centers later develop in the epiphyses, usually around or after birth.
- The epiphyseal plate (growth plate), a band of cartilage between the diaphysis and each epiphysis, is where longitudinal bone growth occurs. Chondrocytes proliferate on the epiphyseal side while bone replaces cartilage on the diaphyseal side.
Bone Growth and Remodeling
Even after bones finish forming, they continue to change throughout life.
- Longitudinal growth continues as long as the epiphyseal plates remain open. During puberty, rising sex hormone levels cause the plates to ossify and close, ending height increase.
- Appositional growth adds bone to the outer surface (via osteoblasts in the periosteum), increasing bone thickness.
- Remodeling is the ongoing, coordinated cycle of osteoclast resorption and osteoblast deposition. It replaces old or damaged bone, reshapes bone in response to mechanical stress, and regulates blood calcium levels.
Hormonal regulation plays a central role in this process:
- Parathyroid hormone (PTH), released when blood calcium drops, stimulates osteoclast activity to release calcium from bone. PTH also increases calcium reabsorption in the kidneys and promotes activation of vitamin D, which enhances calcium absorption in the intestines.
- Calcitonin, released by the thyroid gland when blood calcium is too high, inhibits osteoclast activity and promotes calcium deposition into bone.
These two hormones work in opposition to maintain calcium homeostasis, keeping blood calcium within a narrow, functional range.